|
Morganella has been reported as the cause of up to 3% of bacteremias in a nursing home, arising primarily from either the urinary tract or soft tissue infections ( 56). In a multicenter study of 2084 cases of bacteremia in Britain, Morganella accounted for 1% of cases and 4 deaths ( 46). morganii bacteremia, Kim found that 64% were related to intra-abdominal infections (included biliary infection, liver abscess and peritonitis) ( 38). In a retrospective review of 61 cases of M. morganii bacteremia involved hepatobiliary tract was 22% by Lee report during one-year period ( 41). Morganella could also cause intra-abdominal infections. In a retrospective review of 19 cases of Morganella bacteremia McDermott found that 37% were related to wound infections ( 49). Falagas reported 13 patients (54%) suffered from skin and soft tissue infections in a 4-year period at Greece hospital ( 23). Morganella usually causes skin and soft tissue infections. In a prospective monitoring of all Morganella cultures in a VA microbiology laboratory 60% of isolates were from the urine, 18% from wounds and the remaining 22% from a variety of body fluids or tube drainage ( 49). found Morganella bacteriuria in 19% of weekly specimens with a mean duration of bacteriuria of 3.3 weeks ( 83). In a study of 20 patients with chronic indwelling urinary catheters, Warren et al. Morganella is the fifth leading cause of UTIs in nursing home patients ( 59). Urinary tract infection is the most common clinical infection site. Most often these occur in elderly patients in nursing homes with long-term indwelling catheters ( 84). morganii often involve the urinary tract, skin and soft tissue and hepatobiliary tract ( 42). morganii bacteremia among nosocomial infections in newborns ( 17).Ĭlinical infections due to M. morganii bacteremia is not common and only accounts for 0.69% of bacteremia reported by Lee et al ( 41). morganii bacteremia cases were opportunistic community-acquired infections. morganii is found in the environment and in the intestinal tracts of humans, mammals, and reptiles as part of the normal flora ( 23). The organism has been isolated along with Proteus mirabalis more frequently in patients with diarrhea than in healthy controls ( 57). Morganella morganii was originally thought to be a cause of summer diarrhea. Morganella species are infrequent causes of disease in healthy individuals. Siboniiwith four and three biogroups respectively can be differentiated based on biochemical and genetic features ( 60). Morganella species can ferment mannose and have the enzyme ornithine decarboxylase which Proteus lack ( 24). They can be separated from Proteus species by the lack of swarming activity or gelatin liquefaction or H2S production. Morganella are motile, non-lactose fermenting gram-negative bacteria, which share with Proteus the capacity for urease production and presence of phenylalanine deaminase. defined two subspecies of Morganella ( 33). In 1992 using DNA hybridization Jensen et al. Later in 1943 Fulton would classify these strains into the genus Morganella ( 27). In 1914 he described this bacteria along with two others as Bacterium Columbense ( 12). Independently Castellani isolated a bacterium while studying a case of fever in 1905 in Colombo, Sri Lanka. This bacterium came to be known as Morgan’s bacillus and was later classified as Bacillus morganii ( 55). In 1906 Morgan described a non-lactose fermenting organism in children with summer infantile diarrhea. Proteus and Providencia are the other members of this tribe and share some of the biochemical and clinical characteristics ( 8, 9). 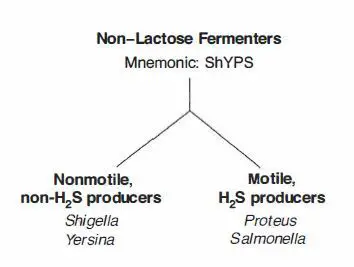
Morganella is the third member of the tribe Proteeae.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
